Abstract
Objective
Drug-induced psychosis is a frequent side–effect in the treatment of advanced Parkinson’s disease (PD). We sought to develop and evaluate a brief instrument for early recognition of drug–induced psychosis in PD.
Methods
We developed the “Parkinson Psychosis Questionnaire” (PPQ), which consists of screening questions for typical early signs and psychotic symptoms in PD and which quantifies the frequency and severity of four clinical categories—sleep disturbances, hallucinations/illusions, delusions and orientation. We performed an internal validation of the PPQ in 50 unselected patients with parkinsonism. The Brief Psychiatric Rating Scale (BPRS) and the “Structurized Clinical Interview” (SCID) for DSM IV were applied to the same patients as external references.
Results
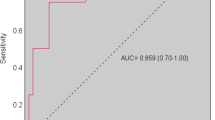
Of 50 subjects, 49 suffered from idiopathic PD and one from probable MSA–P. Hoehn and Yahr stages in “on” ranged from 1.5 to 4. Sensitivity of the PPQ test for drug–induced psychosis according to SCID was 100 % (95 % CI: 73.5%, 100%); while specificity was 92.1 % (95% CI: 78.6%, 98.3 %). The PPQ severity score was highly correlated with BPRS. We derived a linear prediction formula, which transformed PPQ into BPRS scores.
Conclusion
The PPQ appears to be a suitable, and easily administered instrument for early diagnosis of druginduced psychosis in routine PD care. Whether the PPQ could also be a valuable tool for monitoring follow–up studies and therapeutic intervention trials remains to be tested.
Similar content being viewed by others
References
Melamed E, Friedberg G, Zoldan J (1999) Psychosis–impact on the patient and family. Neurology 52(Suppl):14–16
Carter JH, Stewart BJ, Archold PG (1998) Living with a person who has Parkinson’s disease: the spouse’s perspective by stage of disease. Mov Disord 13:20–28
Friedman JH (1991) The management of levodopa psychosis. Clin Neuropharmacol 14:283–295
Goetz CG, Stebbins GT (1995) Mortality and hallucinations in nursing home patients with advanced Parkinson’s disease. Neurology 45:669–671
Goetz CG, Stebbins GT (1993) Risk factors for nursing home placement in advanced Parkinson’s disease. Neurology 43:2227–2229
Doraiswamy M, Martin W, Metz A, Deveaugh–Geiss J (1995) Psychosis in Parkinson’s disease: Diagnosis and treatment. Prog Neuro–Psychopharmacol Biol Psychiatry 19:835–846
Aarsland D, Laarsen JP, Cummings JL, Laake K (1999) Prevalence and clinical correlates of psychotic symptoms in Parkinson’s disease. A communitybased study. Arch Neurol 56:595–601
Wolters EC (1999) Dopaminomimetic psychosis in Parkinson’s disease patients. Neurology 52(Suppl):10–13
Cummings JL (1991) Behavioral complications of drug treatment of Parkinson patients. J Am Geriat Soc 39:708–716
Moskovitz C, Moses H, Klawans HL (1978) Levodopa–induced psychosis: A kindling phenomenon. Am J Psychiatry 135:669–675
Pappert EJ, Goetz CG, Niederman FG, Raman R, Leurgans S (1999) Hallucinations, sleep fragmentation and altered dream phenomena in Parkinson’s disease. Mov Disord 14:117–121
Nausieda PA, Weiner WJ, Kaplan LR, Weber A (1982) Sleep disruption in the course of chronic levodopa therapy: an early feature of levodopa psychosis. Clin Neuropharmacol 5:183–195
Fenelon G, Mahieux F, Huon R, Ziegler M (2000) Hallucinations in Parkinson’s disease – prevalence, phenomenology and risk factors. Brain 123:733–745
Friedman JH, Factor SA (2000) Atypical antipsychotics in the treatment of drug–induced psychosis in Parkinson’s disease. Mov Disord 15:201–211
Friedberg G, Zoldan J, Weizman A, Melamed E (1998) Parkinson psychosis Rating Scale: A practical instrument for grading psychosis in Parkinson’s disease. Clin Neuropharmacol 21:28–284
Sanchez–Ramos JR, Ortoll R, Paulson GW (1996) Visual hallucinations associated with Parkinson’s disease. Arch Neurol 53:1265–1268
Wittchen HU, Wunderlich U, Gruschwitz S, Zaudig M (1997) SKID – Strukturiertes klinisches Interview für DSM IV (deutschsprachige, erweiterte Bearbeitung der amerikanischen Originalversion SCID). Hogrefe Verlag, München
Overall JE, Gorham DR (1988) Introduction – the Brief Psychiatric Rating Scale (BPRS): recent developments. Psychopharmacol Bull 21:97–99
Hoehn M, Yahr M (1967) Parkinsonism: onset, progression and mortality. Neurology 17:427–442
Lang AET, Fahn S (1989) Assessment of Parkinson’s disease. In:Munsat TL (ed) Quantification of neurologic deficit. Butterworths, Boston, pp 285–309
Folstein MF, Folstein SE, McHugh PR (1975) Mini–Mental State. A practical method for grading the cognitive state of patients for clinicians. J Psychiatric Res 12:189–198
Hughes AJ, Daniel SE, Kilford L, Lees AJ (1992) Accuracy of clinical diagnosis of idiopathic Parkinson’s disease. A clinico–pathological study of 100 cases. J Neurol Neurosurg Psychiatry 55:181–184
Gilman S, Low PA, Quinn N, et al. (1999) Consensus statement on the diagnosis of multiple system atrophy. J Neurol Sci 163:94–98
Goetz CG, Leurgans S, Pappert EJ, Raman R, Stemer AB (2001) Prospective longitudinal assessment of hallucinations in Parkinson’s disease. Neurology 57:2078–2082
Brandstaedter D, Lotze J, Spieker S, Ulm G, Oertel WH (2002) Treatment of drug–induced psychosis with quetiapine and clozapine in Parkinson’s disease. Neurology 58:160–161
McKeith IG, Galasko D, Kosaka K, et al. (1996) Consensus guidelines for the clinical and pathological diagnosis of dementia with Lewy bodies (DLB): report of the consortium on DLB international workshop. Neurology 47:673–678
Cronbach LJ (1951) Coefficient alpha and the internal structure of tests. Psychometrika 16:297–333
Bland JM, Altman DG (1997) Cronbach’s alpha. BMJ 314:572
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brandstaedter, D., Spieker, S., Ulm, G. et al. Development and evaluation of the Parkinson Psychosis Questionnaire. J Neurol 252, 1060–1066 (2005). https://doi.org/10.1007/s00415-005-0816-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-005-0816-x