Abstract
Background: Brain imaging studies of major depressive disorder have shown alterations in the brain regions typically involved in episodic memory, including the prefrontal cortex and medial temporal areas. Some studies of major depressive disorder have linked episodic memory performance to treatment response. In this study, we sought to identify brain regions whose activity, measured during the encoding of pictures, predicted symptomatic improvement after 8 weeks of citalopram treatment.
Methods: We included 20 unmedicated depressed patients. These patients performed an episodic recognition memory task during functional magnetic resonance imaging. During the encoding phase, 150 pictures depicting emotionally positive, negative or neutral content were presented, and the participants were required to classify each picture according to its emotional valence. The same 150 pictures were presented, along with 150 new ones, for a recognition task. We asked participants to distinguish the old pictures from the new ones. We assessed symptom severity by use of the 21-item Hamilton Rating Scale for Depression (HAM-D) at baseline and after 8 weeks of citalopram treatment. We performed subsequent memory effect analyses using SPM2 software. We explored the relation between brain activation during successful encoding of pictures and symptomatic improvement.
Results: Patients showed a mean symptomatic improvement of 54.5% on the HAM-D after 8 weeks. Symptomatic improvement was significantly and positively correlated with picture recognition memory accuracy. We also found that the activity of the ventromedial prefrontal cortex and anterior cingulate cortex during successful encoding was significantly correlated with symptomatic improvement. Finally, we found greater activation in the ventromedial prefrontal cortex during the successful encoding of positive pictures in comparison with neutral pictures.
Limitations: During the recognition memory task, 5 participants (among the best responders to treatment) were not included in the valence-specific analyses because they had very few errors. A more challenging task would have allowed the inclusion of most patients.
Conclusion: Different types of functional imaging paradigms have been used to explore whether the activity of specific brain regions measured at baseline is predictive of a better response to treatment in major depressive disorder. Among these regions, the medial prefrontal cortex and anterior cingulate cortex usually show the strongest predictive value. According to our results, the medial prefrontal cortex and anterior cingulate cortex could have an effect on treatment response in major depressive disorder by contributing to the successful encoding of positively valenced information.
Introduction
About 20% of patients with major depressive disorder (MDD) will not adequately respond to pharmacologic treatment.1 The identification of the neural processes implicated in symptomatic improvement in MDD is a clinically relevant challenge for neuroimaging studies. There is a growing body of literature highlighting the importance of memory processes in understanding the course of MDD. Episodic memory deficits are usually found in patients with MDD2,3 and likely represent a premorbid marker of depression.4 In addition, several brain abnormalities have been associated with these memory deficits, including frontal, striatal and temporal blood hypoperfusion5,6 and hippocampal volume reduction.7 Interestingly, memory impairments in MDD have a predictive value for response to future treatment. For example, a recent study involving 30 patients with late-onset depression after 12 weeks of antidepressant treatment found a significant association between the magnitude of symptomatic improvement and several neurocognitive measures, including both verbal and visual memory.8
In another recent study, Johnson and colleagues9 found that the ability to remember positively valenced information predicted a decrease in depressive symptoms in MDD about 9 months after initial evaluation. Additionally, Joormann and colleagues10 observed that depressed patients, unlike healthy controls, were not able to improve a preinduced sad mood by recalling positive events. These results stress the importance of potential alterations in memory processes in the prediction of treatment outcomes in MDD.
Past neuroimaging studies, using both positron emission tomography and functional magnetic resonance imaging (fMRI) techniques, have repeatedly demonstrated that the activity of the rostral anterior cingulate cortex (ACC) usually predicts treatment response in MDD. Some of these studies used experimental paradigms that involved the measurement of brain activity in a resting state,11–18 during the observation of emotional stimuli19 or during inhibitory control.20–22 For example, Davidson and colleagues19 used an emotional activation paradigm involving emotional pictures with positive, neutral or negative valence to predict symptomatic improvement after 8 weeks of venlafaxine treatment. They found that patients who showed more activity in the rostral anterior cingulate cortex during the processing of negative information at baseline also had greater reduction of their depressive symptoms after treatment. Based on the potential role of the rostral ACC in processing conflicting affective responses, the authors suggested that patients who improve may have a greater ability to resolve conflicts between their mood and their expectations of daily living compared with those who did not improve.
In this study, we investigated whether brain activity measured during memory encoding of complex emotional pictures is predictive of the magnitude of treatment response following 8 weeks of citalopram treatment. We used a subsequent memory effect approach, which is particularly effective for extracting brain activity associated with successful encoding of specific types of information.23 Several regions associated with successful memory encoding have been identified, including the medial temporal areas and the lateral and medial areas of the prefrontal cortex.24 At the behavioural level, we hypothesized that symptomatic improvement would be significantly and positively correlated with recognition memory accuracy for complex pictures. At the functional neuroimaging level, we hypothesized that the activity of the medial temporal lobe and prefrontal cortex during successful encoding would be significantly and positively correlated with symptomatic improvement.
Methods
Participants
We recruited 22 patients with unmedicated depression aged 18–59 years, from the Depressive Disorders Program at the Douglas Mental Health University Institute. We excluded patients with a past or current neurologic condition (including head trauma with loss of consciousness) that could impair cognition, current substance abuse disorder (i.e., DSM-IV criteria for substance abuse or dependence within at least 6 months) or a family history of hereditary neurologic disorders. We excluded one patient because of technical issues during scanning and another because of a change in diagnosis (from MDD to bipolar disorder). All other patients met the DSM-IV criteria for MDD. The clinical evaluation included the Structured Clinical Interviews for Axis I and Axis II disorders (SCID-I and SCID-II),25 and the 21-item Hamilton Rating Scale for Depression (HAM-D)26 to assess symptoms severity. Table 1 depicts the demographic, cognitive and clinical data for the 20 patients included in the analyses.
Characteristics of patients with major depressive disorder (n = 20)*
The study was approved by the institutional review boards of the Montreal Neurological Institute and the Douglas Mental Health University Institute. Informed written consent was also obtained from all participants.
Procedure
Depressed patients who agreed to participate and who met our inclusion criteria were scanned within 7 days of their first clinical assessment at the Depressive Disorders Program. Scanning sessions were conducted at the Montreal Neurological Institute. Three days after the scanning session, the patients came to the Douglas Mental Health University Institute to undergo behavioural testing. We estimated full-scale intelligence quotient (IQ) using the Wechsler Abbreviated Scale of Intelligence.27 All patients were then given citalopram orally at an initial dose of 10 mg, which was progressively titrated to a maximum of 50 mg and maintained for at least 8 weeks, with a minimum period of 4 weeks at the full dosage. During the eighth week of treatment, patients were taking, on average, 41 mg of citalopram (standard deviation [SD] 6.41). Citalopram was used monotherapeutically, and no other psychotropic medication was prescribed with the exception of hypnotic medication to treat insomnia (i.e., up to 7.5 mg of zopiclone or equivalent). After the eighth week of treatment with citalopram, we obtained blood samples to measure citalopram blood concentration, and we performed a new HAM-D assessment. This second assessment allowed us to calculate the percentage of symptomatic improvement after 8 weeks.
Experimental task
The patients underwent a picture recognition memory task in the fMRI scanner using an event-related procedure. We selected 300 colour pictures from various sources, mainly the International Affective Picture System (IAPS)28 and the Empathy Picture System (EPS).29 The IAPS consists of an extensive series of more than 400 experimentally validated pictures of people, places and objects representing different affective possibilities. The EPS comprises 12 picture series, each containing 30 pictures depicting people in real-life situations. The EPS picture series are subdivided according to their emotional valence.
The stimuli were divided into 3 conditions based on emotional content: positive, neutral or negative. The memory task was divided in 2 parts: an encoding phase and a recognition memory test. Participants were informed about the structure of the task before the scan; that is, they were told that the pictures presented in the first phase would have to be recognized in a subsequent recognition phase. Hence, the task did not involve incidental encoding of the pictures. During the encoding phase, 150 pictures (50 each of positive, negative and neutral) from 3 pregenerated lists (counterbalanced across participants) were pseudorandomly presented to the participant one at a time. Each picture was presented for 3 seconds, followed by a fixation cross presented for 2 seconds. During the encoding phase, patients performed a picture valence categorization task; that is, they had to determine whether each picture had a positive, negative or neutral valence using a 3-button computer mouse.
During the recognition memory test, 300 pictures were presented, including 150 “previously seen” or “old” pictures and 150 novel pictures. As in the encoding phase, each picture was presented for 3 seconds, followed by a fixation cross presented for 2 seconds. Participants were asked to identify the old and new pictures by clicking on predetermined “old” and “new” buttons. The recognition memory test was conducted over 2 separate fMRI runs, during which 150 pictures (75 old pictures and 75 new ones) were presented. Memory performance accuracy (Pr) was calculated by use of the discrimination index Pr (Pr = H − FA), where H and FA represent hit and false alarm rates, respectively. The Pr index provides an unbiased estimate of the accuracy of the response to old and new items, where higher values correspond to better (more accurate) memory.30 We calculated recognition memory accuracy separately for each emotional valence condition (Pr-Neutral, Pr-Negative and Pr-Positive), as well as for the global memory performance (conditions pooled together: Pr-Global).
After the scanning session, participants performed a picture valence rating task on a laptop computer. To get more precise and idiosyncratic ratings from participants, each picture was accompanied by a continuous line with the label “very negative” at the left end of the line and the label “very positive” at the right end. Participants were told that the middle of the line was associated with neutrality. Using a mouse, participants moved an arrow on this line and clicked the left button once the arrow was well-positioned according to the emotional valence of the picture. The continuous line was in fact an ordinal scale ranging from “1” (very negative) to “323” (very positive).
Image acquisition
We acquired fMRI data at the Montreal Neurological Institute on a 1.5-T Siemens Sonata whole-body system equipped with a standard head coil, using gradient echo planar imaging sequences. A vacuum cushion stabilized the participant’s head. Stimuli were generated by an IBM PC laptop computer running E-Prime (Psychology Software Tools) and projected via an LCD projector and mirror system. A mouse connected to the computer recorded the participants’ responses. Functional T2*-weighted images were acquired with blood oxygenation level–dependent (BOLD) contrasts (3 functional runs of 278 volumes, repetition time 2750 ms, echo time 50 ms, flip angle 90º, field of view 256 mm, matrix 64 × 64), covering the entire brain (30 interleaved slices parallel to the anterior–posterior commissural plane, in plane resolution 4 × 4 mm, 4-mm thickness). Following the functional session, a high-resolution T1-weighted anatomic volume was acquired using a gradient echo pulse sequence (22 ms, echo time 9.2 ms, flip angle 30º, voxel size 1 × 1 × 1 mm3). The scanning session lasted about 1.5 hours, including set-up time.
Statistical analyses
Behavioural data
We verified normal distributions for Pr-Neutral, Pr-Negative, Pr-Positive, Pr-Global, symptomatic improvement and valence ratings of each emotional condition. Normality correction was not necessary for any of these variables. Repeated-measures analyses of variance (ANOVAs) with the emotional valence condition (positive, negative and neutral) as the within-subject factor were conducted for the following variables: percent accuracy and reaction times during the emotional valence categorization task, memory accuracy and reaction times during the recognition memory task and the emotional valence ratings. We tested for sphericity and found the results of the Mauchly sphericity test significant for all variables (except reaction times during the recognition memory task); thus, we applied the Greenhouse–Geisser correction. We conducted Pearson’s coefficient correlation analyses to verify potential links between symptomatic improvement, Pr-Global and memory accuracy for each valence condition (Pr-Positive, Pr-Negative and Pr-Neutral). We performed the statistical tests using SPSS for Windows (version 15.0).
Functional MRI data
We analyzed the fMRI data using Statistical Parametric Mapping (SPM2, Wellcome Department of Cognitive Neurology). We performed image preprocessing according to a standard procedure.31 The images were time-corrected to take into consideration differences in sampling times of different slices, realigned to the first volume to correct for interscan movement, spatially normalized to the Talairach standard space32 and smoothed with a 10-mm full-width at half-maximum Gaussian kernel. Low-frequency temporal drifts were removed by applying a high-pass filter. We analyzed the data under the general linear model, in which individual events were modelled by a synthetic hemodynamic response function. We conducted subsequent memory effect analysis on brain activity sampled during the encoding phase. Event types were modelled using the participant performance rates obtained during the recognition memory test. Only pictures that were accurately categorized in the appropriate emotional valence condition during the viewing phase were included in the fMRI analyses.
The feasibility of the subsequent memory effect analysis relied on minimal errors in each condition of interest. For instance, a “subsequently forgotten” event type (e.g., positive pictures subsequently forgotten during the recognition phase) required some errors from each participant. We established a minimum cutoff of 5 errors (or events) per condition. The initial subsequent memory effect analysis involved the contrast between all pictures (positive, negative and neutral pictures) subsequently remembered (“hits”) and all pictures subsequently forgotten (“misses”). This analysis permitted the identification of the brain regions associated with successful encoding of complex pictures, regardless of their emotional valence (1-sample t test, p < 0.001, uncorrected). Further, we correlated the brain activity extracted from this contrast (individual contrast image all pictures hits minus all pictures misses) with the percentage of symptomatic improvement obtained from each participant. This second analysis identified the brain regions whose activity during successful encoding was also predictive of symptomatic improvement (simple regression analysis at p < 0.005, uncorrected).
To test for specific valence effect, we also conducted a subsequent memory effect analysis for each emotional valence condition (positive, negative and neutral). These 3 extra subsequent memory effect analyses allowed us to identify the brain regions associated with the successful encoding of pictures from each type of valence condition: positive pictures hits minus positive pictures misses, negative pictures hits minus negative pictures misses, and neutral pictures hits minus neutral pictures misses (1-sample t tests, p < 0.005, uncorrected). We also conducted paired t tests to directly compare the subsequent memory effect of both emotional conditions with subsequent memory effect of neutral pictures (subsequent memory effect [SME] positive v. SME neutral, SME negative v. SME neutral at p < 0.005, uncorrected). These analyses identified which brain regions were specifically involved in successful encoding of positive (or negative) information compared with neutral information. Five participants who did not reach the minimum error cutoff required for each valence condition (5 errors) were not included in these additional valence-specific subsequent memory effect analyses.
Based on the results obtained from the second analysis (all pictures hits minus all pictures misses correlated with symptomatic improvement), we extracted for each participant the contrast estimates (β weights) of the BOLD signal in the right rostral anterior cingulate cortex (x = 16, y = 30, z = 17) and the left ventromedial prefrontal cortex (PFC) (x = −12, y = 46, z = −6) for the contrast of all pictures hits minus all pictures misses. Then, to control for potential confounds, we conducted 2 separate multiple regression analyses in SPSS using the symptomatic improvement as the dependent variable and age, education, sex, estimated IQ, HAM-D baseline, Pr-Global and rostral ACC activity (contrast estimates of the BOLD signal) and ventromedial PFC activity as independent variables. The goal of these analyses was to calculate the explicative variance associated with each independent variable for symptomatic improvement following 8 weeks of citalopram therapy. We also correlated rostral ACC and ventromedial PFC activity with global memory accuracy (Pr-Global), as well as with memory accuracy for each valence condition.
Results
Behavioural data
For the valence ratings (positive, negative and neutral), ANOVA showed a significant effect of valence (F1.23,38 = 335.63, p < 0.001, Table 2 ). Pairwise comparisons with Bonferroni adjustment showed a significant difference between each valence condition (negative < neutral < positive, p < 0.001). Regarding the percentage of accuracy in the emotional valence categorization task, ANOVA revealed a non-significant effect of valence (F1.32,38 = 3.67, p = 0.06). Another ANOVA was conducted for reaction times during the emotional valence categorization task (positive valence: mean 1237 [SD 182] ms; negative valence: mean 1313 [SD 173] ms; neutral valence: mean 1400 [SD 183] ms) and showed a significant effect of valence (F1.49,38 = 7.98, p = 0.004). Pairwise comparisons demonstrated a significant difference in reaction times only between the positive and neutral valences (p < 0.05), suggesting that MDD patients needed more time to categorize neutral pictures than positive ones.
Results of a picture valance rating task for patients with major depressive disorder
For recognition memory accuracy (index Pr), ANOVA showed a significant effect of valence (F1.28,38 = 10.15, p = 0.002). The results of pairwise comparisons showed a significant difference in recognition memory accuracy only between positive and neutral valence conditions (p = 0.001) and between positive and negative valence conditions (p < 0.001). Thus, MDD patients were significantly less accurate in recognizing positive pictures compared with neutral or negative ones. An ANOVA performed for reaction times during the recognition task (positive valence: mean 1372 [SD 165] ms; negative valence: mean 1408 [SD 146] ms; neutral valence: mean 1288 [SD 169] ms) showed a significant effect of valence (F2,38 = 29.08, p < 0.001). Pairwise comparisons showed significant differences between neutral and negative valence conditions (p < 0.001) and between neutral and positive valence conditions (p < 0.001). Neutral pictures were remembered faster than emotional ones.
Among the 20 patients included in the study of recognition memory accuracy and symptomatic improvement, we found that symptomatic improvement was significantly and positively correlated with Pr-Global (r = 0.53, p = 0.015), Pr-Negative (r = 0.51, p = 0.021) and Pr-Positive (r = 0.49, p = 0.028). No significant difference was found for Pr-Neutral (r = 0.43, p = 0.06).
Functional MRI
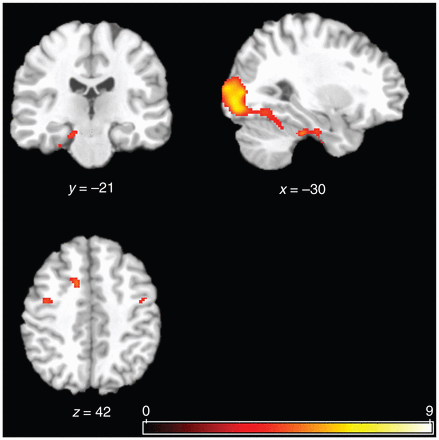
We initially identified the brain regions involved in the successful encoding of complex pictures. We found significant bilateral activation in the middle occipital gyri (Brodmann areas [BA] 18 and 19), thalami and bilateral precentral gyrus (BA 6). We also found significant activation in the right fusiform gyrus (BA 37), left dorsal anterior cingulate cortex (BA 32), left parahippocampal gyrus (BA 35), right amygdala and left inferior occipital gyrus (BA 19; Table 3 and Fig. 1).
Brain activity associated with successful encoding of complex pictures (contrast: all pictures hits minus all pictures misses). p < 0.001, uncorrected; 10 voxels was the minimum cluster size.
Results for the subsequent memory effect analyses*
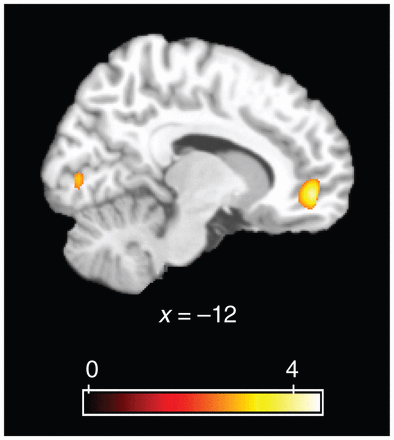
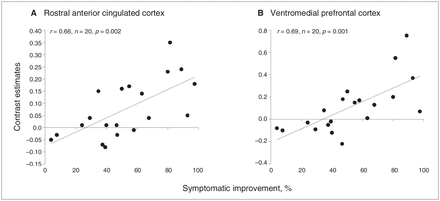
Table 3 and Figure 2 summarize the results from the correlation between brain activity during successful encoding of complex pictures and symptomatic improvement. We found 4 clusters in the frontal lobe that were significantly and positively correlated with symptomatic improvement: left superior frontal gyrus (BA 9), left ventromedial prefrontal cortex (BA 10), right rostral ACC (BA 24/32) and right superior frontal gyrus (BA 6). No brain activation was negatively correlated with symptomatic improvement. Figure 3A shows the correlation between rostral ACC activity (contrast estimates for the contrast of all pictures hits v. all pictures misses) and symptomatic improvement. Figure 3B shows the correlation between ventromedial PFC activity and symptomatic improvement.
Brain regions where activity generated by successful encoding of complex pictures (contrast: all pictures hits minus all pictures misses) was significantly correlated with the symptomatic improvement after 8 weeks of antidepressant treatment. p < 0.005, uncorrected; 10 voxels was the minimum cluster size.
Contrast estimates for the contrast of all pictures hits minus all pictures misses correlated to symptomatic improvement for the peak voxel in the (A) right rostral anterior cingulate cortex (x = 16, y = 30, z = 17) and (B) ventromedial prefrontal cortex (x = −12, y = 46, z = −6).
The contrast of positive pictures hits minus positive pictures misses revealed significant activation in the left middle occipital gyrus (peak voxel: x = −56, y = −70, z = 4, BA 37, t = 6.38, cluster size = 2298), right inferior temporal gyrus (x = 50, y = −68, z = 10, BA 37, t = 5.02, cluster size = 2548), left superior frontal gyrus (x = −22, y = 14, z = 44, BA 8, t = 5.96, cluster size = 341) and left VMPFC (x = −12, y = 50, z = −10, BA 10, t = 4.11, cluster size = 42). For the contrast of negative pictures hits minus negative pictures misses, we found significant activation in the right fusiform gyrus (x = 46, y = −64, z = −14, BA 19, t = 6.00, cluster size = 307), left inferior occipital gyrus (x = −40, y = −86, z = 4, t = 5.76, BA 19, cluster size = 354), left middle occipital gyrus (x = −26, y = −96, z = 6, BA 18, t = 4.90, cluster size = 170), right hippocampus (x = 36, y = −26, z = −10, t = 5.01, cluster size = 65) and left rostral ACC (x = −20, y = 40, z = 4, BA 32, t = 4.32, cluster size = 36).
The contrast of neutral pictures hits minus neutral misses revealed significant activation in the bilateral precentral gyri (right: x = 40, y = 2, z = 36, BA 6, t = 4.56, cluster size = 95; left: x = −54, y = −6, z = 30, BA 6, t = 4.38, cluster size = 68) and bilateral insula (right: x = 52, y = −20, z = 16, BA 41, t = 3.67, cluster size = 106; left: x = −38, y = −2, z = 14, BA 41, t = 4.21, cluster size = 83).
The paired t test for SME positive minus SME neutral showed significant activation in the right middle temporal gyrus (BA 37), left middle and superior occipital gyri (BA 19), right superior frontal gyrus (BA 8), bilateral ventromedial PFC (BA 10) and right fusiform gyrus (BA 37). This contrast identified brain regions that were significantly involved in successful encoding of positive versus neutral pictures. The brain regions significantly involved in successful encoding of negative versus neutral pictures included the right hippocampus, left superior parietal lobule (BA 7) and left middle occipital gyrus (BA 18; Table 3).
The multiple regression analysis that included rostral ACC activity as an independent variable revealed a significant model explaining the symptomatic improvement following an 8-week citalopram treatment (F1,15 = 13.61, p = 0.002, adjusted R2 = 0.40). The only significant variable included in this model was rostral ACC activity. No other variable significantly explained symptomatic improvement. The multiple regression analysis that included ventromedial PFC activity as an independent variable showed a significant model explaining symptomatic improvement (F4,15 = 12.95, p < 0.001, adjusted R2 = 0.72). Significant variables included in this model were ventromedial activity (R2 variation = 0.47 and standardized β = 0.57, p = 0.001), the HAM-D baseline (R2 variation = 0.14, standardized β = 0.38, p = 0.007), Pr-Global (R2 variation = 0.23, standardized β = 0.40, p = 0.011) and sex (R2 variation = 0.03, standardized β = −0.28, p = 0.042).
Finally, among the 20 participants, rostral ACC activity (contrast estimates extracted from the contrast all pictures hits v. misses) was significantly correlated with memory accuracy for all pictures combined (Pr-Global: r = 0.53, p = 0.017), as well as for positive pictures (Pr-Positive: r = 0.52, p = 0.018) and negative pictures (Pr-Negative: r = 0.46, p = 0.040). The results were nonsignificant for the neutral pictures (Pr-Neutral: r = 0.43, p = 0.06). Interestingly, ventromedial PFC activity (contrast estimates extracted from the contrast all pictures hits vs. all pictures misses) was only significantly correlated to memory accuracy for the positive pictures (Pr-Positive: r = 0.49, p = 0.029). There was no significant correlation between ventromedial PFC activity and memory accuracy for all pictures combined (Pr-Global: r = 0.41, p = 0.07), negative pictures (P-Negative: r = 0.35, p = 0.13) or neutral pictures (P-Neutral: r = 0.27, p = 0.24).
Discussion
Our main goal was to investigate whether brain activity during successful memory encoding of complex pictures predicted symptomatic improvement following 8-week antidepressant therapy in patients with MDD. Our initial subsequent memory effect analysis identified the brain regions involved in the successful encoding of complex pictures. The results of this analysis were consistent with the literature33–35 and included key regions typically linked to the memory encoding of visual stimuli, such as the hippocampal/parahippocampal areas, fusiform gyrus, amygdala, dorsal PFC and the occipital lobe. Hence, our initial analysis provided some support for the validity of our subsequent memory effect paradigm.
Consistent with our behavioural hypothesis, we found that a greater recognition memory for complex pictures was significantly and positively correlated with symptomatic improvement at follow-up. We also found a significant relation between PFC activity at baseline, including both left ventromedial PFC (x = −12, y = 46, z = −6) and right rostral ACC (x = 16, y = 30, z = 17), and the magnitude of symptomatic improvement after 8 weeks. In fact, all of the brain regions whose activity during successful encoding was significantly correlated with symptomatic improvement were located in the frontal lobe. This is not surprising given the fact that our memory task did not involve incidental encoding. The increased activity of the frontal areas during successful memory encoding may reflect the use of a specific encoding strategy or increased use of attentional or executive resources during the processing of picture content.36 The significant relation between frontal activity and symptomatic improvement may also be related to the concept of interference resolution. Indeed, the patients who improved the most may have been able to both accurately rate the pictures during the categorization task and at the same time minimize the interference from the emotional and cognitive elements of the categorization task on the encoding processes. This capacity to deal with interference may in turn have a beneficial effect on the improvement of symptoms.
If recognition memory performance is significantly associated with symptomatic improvement, one could also expect to find a significant relation between medial temporal activity during successful encoding and symptomatic improvement, given the undisputed role of medial temporal areas in episodic memory.34 However, there was no significant correlation between medial temporal activity and symptomatic improvement. The lack of a significant correlation may indirectly suggest that the link between frontal activity and symptomatic improvement is not only driven by memory. For example, a well-known study by Mayberg and colleagues,15 as well as several subsequent studies, linked increased rostral ACC activity to symptomatic improvement in a resting state, suggesting that this region is particularly important in symptomatic improvement regardless of the involvement of memory-related processes. It is also possible that the increased frontal activity during successful encoding in those who improved reflects greater frontal functioning in general (i.e., greater executive/attentional resources). Consistent with this, Paller and Wagner34 suggested that the pre-frontal areas influence encoding by modulating posterior neocortical processing and by regulating input to the medial temporal areas. It is possible that the executive and/or affective aspects of memory processing, mainly subserved by the prefrontal cortex, contribute to symptomatic improvement and that storage mechanisms much more associated to the medial temporal lobes are less prone to directly contribute to symptomatic improvement.
Multiple regression analyses supported the main findings of this study. In both analyses, medial PFC activity (ACC in one analysis and ventromedial PFC in the other) was the best predictor of the explained variance of symptomatic improvement after 8 weeks of citalopram treatment. The multiple regression analysis that included rostral ACC activity found this variable to be the only significant predictor of symptomatic improvement, supporting the predictive value of rostral ACC over confounding variables. Not surprisingly, the HAM-D score at baseline was also a good predictor of the explained variance of symptomatic improvement in the ventromedial PFC model, possibly because patients with more severe symptoms had more potential for improvement. This model also included the recognition memory accuracy Pr-Global, which was consistent with our hypothesis that better memory would be associated with better symptomatic improvement.
Role of the rostral ACC and ventromedial PFC in treatment response to MDD
Past neuroimaging studies, using both positron emission tomography and fMRI techniques, have shown that rostral ACC activity usually predicts treatment response in patients with MDD. Davidson and colleagues19 found that patients who showed more activity in the left rostral ACC (peak voxel: x = 12, y = 34, z = 14) during the processing of negative information at baseline also showed greater reduction in depressive symptoms after treatment. In another recent study, Langenecker and colleagues21 measured rostral ACC activation using fMRI in 20 depressed patients during the execution of an inhibitory control task before 10-week citalopram treatment. They found a significant positive correlation between the magnitude of symptomatic improvement after 10 weeks and the activity in the dorsolateral prefrontal cortex, ventromedial PFC, amygdala, nucleus accumbens and insula in successful inhibitory trials. In addition, they found that symptomatic improvement was positively correlated with left dorsal ACC (peak voxel: x = −3, y = 22, z = 57) only in unsuccessful inhibition trials (i.e., commissions). They suggested that patients with greater symptomatic improvement may have a greater capacity to detect errors compared with patients who showed reduced symptomatic improvement.
It is interesting to note that we have replicated the main result obtained in past studies — that is, the significant link between prefrontal activity at baseline and symptomatic improvement — using a different neuroimaging paradigm involving subsequent memory effect analyses. The exact nature of the contribution of the ACC and ventromedial PFC for symptomatic improvement is unclear given the different functional tasks that have been used in past studies.15,19,21 Multiple functions have been attributed to the ACC37 and ventromedial PFC,38 including affective processing, inhibitory control and memory encoding. It seems that regardless of the type of task during scanning, depressed patients with greater activation in the ACC and ventromedial PFC consistently show a significant improvement of depressive symptoms after treatment. Moreover, the fact that medial PFC resting state activity is typically linked to symptomatic improvement15 could suggest that there is no single function of this brain area to explain the beneficial impact on symptomatic improvement. Different functions of the medial PFC, including inhibitory control, affect processing and memory encoding, seem to act at different levels in bettering symptomatic improvement. The main findings of the current study contribute to the field by suggesting genuine associations between ACC and ventromedial PFC activity during successful encoding and symptomatic improvement in MDD. This was also supported by the significant correlations between the activity of the rostral ACC and ventromedial PFC and recognition memory accuracy (Pr-Global).
Does the relation between ACC/ventromedial PFC activity and symptomatic improvement involve increased processing of emotional information?
Symptomatic improvement was significantly and positively correlated with the global recognition memory accuracy (Pr-Global), which is consistent with the findings of Marcos and colleagues,8 who reported that verbal and visual memory impairments predict reduced symptomatic improvement in MDD patients after treatment. Moreover, exploring the relation between symptomatic improvement and recognition memory for each valence condition separately revealed that only the emotional conditions (positive and negative) showed significant correlations, although a trend was present for the neutral condition. Our finding that increased recognition memory for emotional pictures predicted better symptomatic improvement is consistent with the results of Johnson and colleagues,9 who found that depressed patients who remembered a greater proportion of positive words endorsed as self-descriptive also had a better symptomatic improvement after 9 months of treatment. Thus, at a behavioural level, there is growing evidence that the capacity to encode and retrieve emotional information favours clinical improvement during treatment. Interestingly, the subsequent memory effect analysis of positive pictures (positive hits v. positive misses) revealed significant activation of the ventromedial PFC, whereas the subsequent memory effect analysis for negative pictures (negative hits v. negative misses) showed a significant activation of the rostral ACC. These regions were not significantly involved during successful encoding of neutral pictures (neutral hits v. neutral misses). Moreover, the activity of the rostral ACC was significantly correlated with memory accuracy for both emotional conditions but not for the neutral condition. Ventromedial PFC activity appeared to be even more specific to the encoding of positively valenced information, as it was significantly correlated only with memory accuracy for positive pictures. This was further supported by the direct comparison of the subsequent memory effect for positive pictures and for neutral pictures, showing that successful encoding of positive pictures requires specific involvement of the ventromedial PFC compared with neutral pictures.
The medial PFC as a whole is well known for its role in emotional processing.37,39,40 Likewise, the dorsomedial PFC (including dorsal ACC) is a key region involved in cognitive aspects (e.g., attention to emotion, appraisal/identification of emotion) of emotional processing.40,41 The ventral regions of the ACC and PFC have also been associated with the production of affective states.42 Several studies have found significant correlations between ventromedial PFC activity and subjective hedonic experience for different types of positive stimuli.43–46 Thus, it is not surprising that the ventromedial PFC was associated with successful encoding of positive information. The ventromedial PFC could modulate encoding through increased processing of positive information. Clinically, our results could suggest that depressed patients who have a greater capacity to process and remember positive events in their life will eventually show better treatment response. These patients might also be less prone to ruminate on negative thoughts.
An alternative hypothesis relates to apathy in MDD patients. Apathy is a common symptom of MDD, marked by a joyless mental state, disinterest in almost all areas of life and indifference or suppression of a large range of emotions. Considering this, it is quite likely that MDD patients with more severe apathy symptoms show greater impairment in the processing of emotional information, which in turn alters brain activation and memory performance for emotional conditions. These patients may also show the worst symptomatic improvement. Conversely, patients with less severe apathy may be more efficient in processing emotional information and may show greater symptomatic improvement. An apathy measure would have provided additional insight into our understanding of the affective processes involved in symptomatic improvement in MDD.
We propose 2 clinical implications of our findings. First, the function of the ACC/ventromedial PFC could provide a useful prediction of antidepressant response and, by extension, increase the rate of treatment success in MDD. This is especially relevant because up to 50% of depressed patients do not respond to the first antidepressant given,47 and nonresponse to treatment is associated with significant distress.48 Likewise, having a reliable response predictor could lead to a better “fine-tuned” selection of specific and/or individually tailored therapeutic interventions. This could result in patients being less likely to be exposed to ineffective treatments. Second, and perhaps more interestingly, new psychosocial and/or somatic interventions could be developed49 to target the emotional memory deficits seen in patients with MDD and the underlying patterns of rostral ACC/ventromedial PFC activation.
Limitations
We excluded 5 participants from the valence-specific fMRI analyses because they made a limited number of errors during the recognition memory task. A related problem was the relatively low minimum cutoff of 5 errors (or events) per condition that we arbitrarily set for our fMRI analyses. Having only 5 trials or events to define a “subsequently forgotten” condition is less than ideal. A more challenging task would have generated a larger number of errors across the different valence conditions and across participants, and, consequently, would have prevented us from excluding a significant number of participants from our sample and defining event types with a small number of trials.
Another important limitation of the study is the lack of a control group. Having data from healthy controls would have facilitated the interpretation of the behavioural and fMRI results. The approach of our study, as in many studies,16,20,50,51 was to compare the most improved patients with the least improved. An important question, still pending because of the lack of a control group, is whether MDD patients who eventually responded to treatment were more or less similar to healthy individuals. Do the brain regions predicting symptomatic improvement reflect normal brain activity in those who improve or brain abnormalities linked to an adaptive response favouring the outcome? Classic studies measuring resting state activity at baseline11,15 have found, for example, increased ACC activity in treatment responders compared with nonresponders and controls. These results support the idea of a brain abnormality, reflecting an adaptive response in MDD patients who later improve. A direct comparison with a control group in our study would have clarified the presence of abnormal brain activity in our patients who improved. At the behavioural level, the presence of a control group would have revealed whether or not our MDD patients who improved showed memory deficits. Despite the lack of a control group, our neuroimaging data remain interpretable but must be treated cautiously. Future studies should incorporate a control group.
Conclusion
The results of the present study support the crucial role of the rostral ACC and ventromedial PFC in clinical improvement in MDD. Furthermore, a significant positive correlation between accuracy of recognition memory for positive information and symptomatic improvement highlights the potential effect of emotional memory deficits in symptomatic recovery in MDD. We suggest that a greater engagement of the ventral areas of the medial PFC may favour the successful encoding of positive information, which in turn could have a beneficial effect on treatment response in MDD. A greater processing efficiency of positively valenced information at baseline in patients with MDD may thus be a cognitive hallmark of subsequent improvement with treatment.
Acknowledgements
This study was supported by a Canadian Institutes of Health Research (CIHR) grant to Dr. Lepage (no. 53280) and Dr. Turecki (no. MOP-68824). Mr. Harvey was supported by fellowships from Fonds de la recherche en santé and CIHR. We thank Daniel Lalande from Laval University for proofreading earlier versions of this paper and Lisa Boucher, Maxime Plante and Thomas Howells for final linguistic revisions.
Footnotes
Drs. Turecki and Lepage share senior authorship of this article.
Competing interests: None declared for Drs. Roy, Turecki, Berlim and Mr. Harvey, Mr. Mamdani and Ms. Beaulieu. Dr. Lepage has received honoraria from Janssen-Ortho and Lilly. He has received payment for the development of educational presentations from CD-Pharma and has received travel/accommodations expenses from Janssen-Ortho.
Contributors: Drs. Roy and Lepage and Mr. Harvey designed the study. Dr. Berlim and Mr. Harvey, Mr. Mamdani and Ms. Beaulieu acquired the data, which Drs. Roy, Berlim, Turecki and Lepage and Mr. Harvey analyzed. Dr. Roy wrote the article, which all other authors reviewed. All authors approved the final version submitted for publication.
- Received January 28, 2009.
- Revision received July 29, 2009.
- Revision received November 25, 2009.
- Revision received January 14, 2010.
- Accepted January 15, 2010.